At Baltimore Vascular Care in Owings Mills, patients are the heart of our center. We take the time to understand your needs, family history and lifestyle in order to provide personalized vascular care.
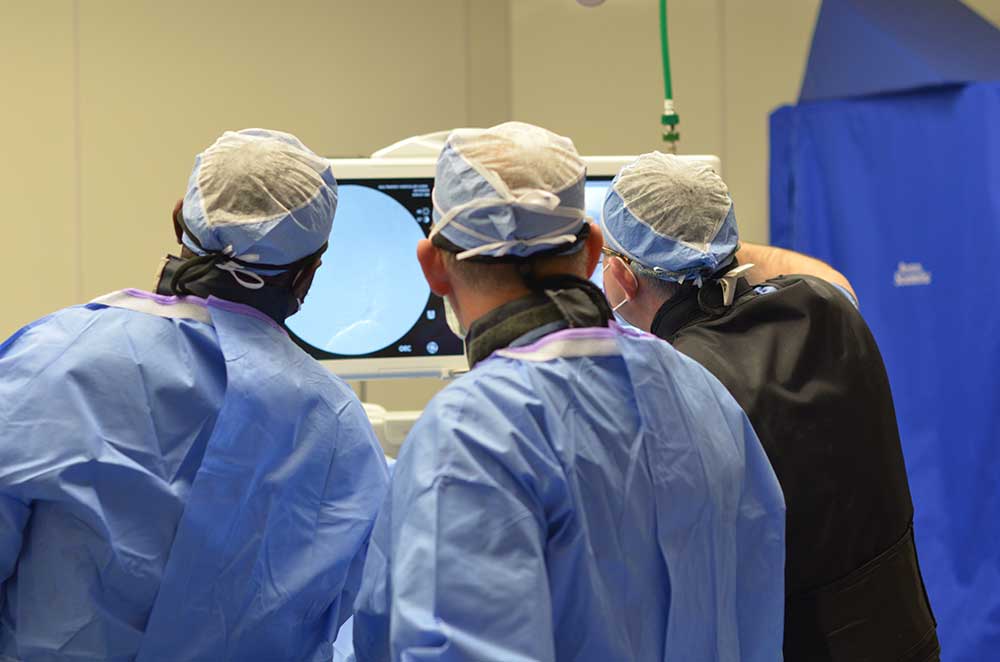
We provide a full range of vascular services using the latest technology backed by the experience of our highly trained physicians, nurses and staff. We take our commitment to excellence in vascular care as seriously as the conditions that we treat. This commitment to excellence in vascular care has made us one of the most trusted vascular centers in the greater Baltimore area.
We use a minimally invasive approach to treating patients in a caring and timely manner. Services we provide include uterine fibroid embolization, diagnosis and treatment of peripheral artery disease (PAD), varicose vein treatments, treatment of varicoceles, interventional oncology, in addition to dialysis access management.
We’re committed to superior service:
At Baltimore Vascular Care, patients can expect:
- Prompt appointments: Same day/next day appointments are available to our ESRD patients. At our center, patients avoid the complexities of a hospital admission and resume normal activities, with minimal disruption.
- Exceptional patient care: Every patient is treated with special attention to their comfort, their time, and their needs. We make every effort to ensure our patients are kept comfortable and well-informed.
- Efficient and customized communication: Post-procedure reports are sent immediately, and comprehensive reports follow within 24 hours after the procedure. We partner with your physicians, coordinating your vascular care.
- Educational programs: We promote patient education, for we believe that knowledge is the key to staying well. We provide opportunities for patients to enhance their understanding of their vascular condition and to be empowered.
If you are a current patient, we thank you for entrusting your vascular needs to Baltimore Vascular Care. If you are a new patient, we welcome you to experience the personal touch that our center provides.
Baltimore Vascular Care is a proud member of the Azura Vascular Care network of outpatient vascular centers located throughout the United States. We partner with the top local vascular care experts to deliver best-in-class patient care, support and service excellence in each and every center.
Azura Vascular Care, working every day to deliver far more than our patients expect, bringing dedicated care ever closer to you.